Female Fertility
If you’ve been trying to conceive for months, or perhaps years, you may be feeling a little deflated and frustrated.
Unfortunately, having problems falling pregnant is not an uncommon problem. In fact, around 1 in 6 couples of reproductive age have trouble conceiving.
There are a number of different reasons why some women are unable to conceive - around 40% of these are because of common gynaecological issues. The good news is that in most cases, there are treatments available to resolve the problem in order to achieve pregnancy.
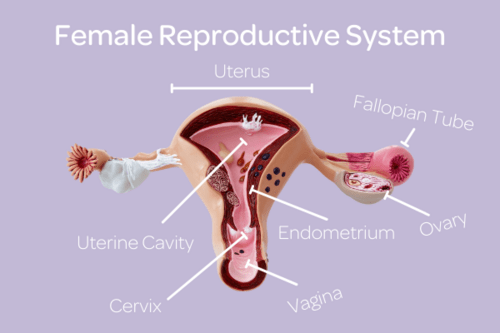
Female Reproductive System
The female reproductive system is a complex system controlled by hormones released by both the brain and ovaries, causing the development and release of eggs during ovulation.
In order to fall pregnant naturally, a woman needs the following reproductive functions:
- Ovulation occurs, producing an egg each month
- A receptive uterus, with the lining of the uterus (the endometrium) thickening to get ready for implantation
- An open pathway for the sperm and egg to meet in the fallopian tubes
Below is an overview of common factors that affect female fertility and reproduction, as well as helpful tools and FAQ’s you may find helpful if you are currently trying to conceive.
If you are having trouble falling pregnant, a Queensland Fertility Group Fertility Specialist can help with investigations and treatment. All of our doctors are expert gynaecologists and/or obstetricians who have undertaken additional training and specialise in fertility. Feel free to get in touch with us to book a consultation, by calling 1800 111 483 or by filling out the form below.
Use our self-assessment tool to check your symptoms
By answering 7 simple questions, this tool is designed to give you an indication of whether there are any factors that might be affecting your chance of falling pregnant and whether you should consider seeking the advice of a fertility specialist for further assessment. Take the female fertility assessment >
Age
A woman’s age is the single most important factor affecting a couple’s chances of conceiving, as her egg quality and reserve starts to rapidly decline after the age of 35. A woman is born with all the eggs she will ever have and from birth this reserve begins to decline, with a very large drop in numbers in her late 30s. At 25 years old, a woman has around a 20% chance of conceiving naturally in any given month. At 35 years old, this has dropped to around 15%, and by 41 years old the chance of conceiving naturally is only around 3%. Read more about age and fertility »
Endometriosis
Endometriosis is a condition where the tissue that normally lines the inside of the uterus – the endometrium – grows outside of the uterus. It often causes painful periods or pain during intercourse, however the severity of the pain experienced is not a reliable indicator of the extent of the condition. Other symptoms include occasional heavy periods or bleeding between periods. Endometriosis can be treated with hormones or with surgery. If the fallopian tubes have been damaged, IVF may be recommended. Read more about endometriosis »
Ovulation problems
Anovulation is the absence of ovulation. The absence of menstruation cycles (amenorrhoea) can be an indicator that ovulation is not occurring. Irregular or unreliable ovulation can cause irregular periods. A common cause of ovulation problems is Polycystic Ovarian Syndrome (PCOS). There are a range of treatments for anovulation from the minimally-invasive, such as fertility medication to induce ovulation, to more involved treatments such surgical procedures, IVF or using donor eggs.
Hyperprolactinemia is the presence of abnormally high levels of the hormone prolactin in the blood. This can stop ovulation (anovulation) from occurring and cause the production of breast milk in non-pregnant women. It can be caused by a number of factors including diseases affecting the hypothalamus and pituitary gland, thyroid disorders, and some prescription medications. Hyperprolactinemia can be treated with drugs to correct hormone imbalances or to induce ovulation, and sometimes surgery to remove pituitary tumours.
Read more about ovulation »
Polycystic Ovarian Syndrome
PCOS (Polycystic Ovarian Syndrome) is a common hormone problem, and one of the leading causes of infertility in women. The term ‘polycystic ovaries’ describes the appearance of the ovaries on an ultrasound scan – ovaries appear to contain many small follicles on an ultrasound scan, described as ‘polycystic’. The dominant follicle, where the egg matures, may not develop as easily, and many of the small follicles will produce varying levels of hormones. Symptoms include irregular periods or no periods at all, heavy yet infrequent periods, increased hair growth, acne, and obesity.
There are several ways to treat PCOS, depending on the severity of the condition. These include weight loss – exercise and a change of diet alone could have a significant impact – or ovulation inducing drugs such as Clomiphene (Serophene or Clomid) or Letrozole can be used to stimulate the ovaries. In severe cases, IVF treatment may be necessary to achieve pregnancy. Read more about PCOS »
Fibroids
Fibroids are lumps of uterine cell tissue or tumorous muscle that grow around and inside the uterus.
Fibroids are very common – up to 80% of women have at least one fibroid – and they typically pose no other threat to your health. Fibroids may be in the uterine wall (intramural fibroids), on the outer surface of the uterus (subserosal fibroids), or protruding into the cavity of the uterus (submucosal fibroids). Read more about Fibroids »
Pelvic inflammatory disease
Pelvic inflammatory disease (PID) is an infection of the female’s upper reproductive organs. It usually occurs when sexually transmitted organisms spread from the vagina to the uterus, fallopian tubes and/or ovaries. It is most often caused by gonorrhoea or chlamydia. It may also be caused by bacteria being introduced into the uterus with the insertion of Intrauterine Devices (IUDs) for birth control, or after miscarriage or pregnancy. Some women do not experience any symptoms while others experience painful or difficult urination, cramps, excessive or irregular bleeding, and fever. Depending on the severity of the disease, treatment may involve antibiotics or surgery.
Premature ovarian failure
Premature ovarian failure, or early menopause, is where a woman’s ovaries stop ovulating before the average age of menopause (between 45 and 55). Women with impending premature ovarian failure may experience irregular or occasional periods, yet some still fall pregnant. Some women reach a complete premature menopause and stop having periods by the age of 40. These women can longer become pregnant.
Symptoms of premature ovarian failure are similar to that of menopause, such as hot flashes, night sweats, vaginal dryness, irritability or difficulty concentrating, and decreased sexual desire. In many cases the cause of POF is unknown; however genetics, toxins, autoimmune disorders, cancer and surgery are all believed to cause POF.
Restoring oestrogen levels in women with premature ovarian failure helps prevent some complications, such as osteoporosis, but infertility is harder to treat with most patients requiring IVF (with donor eggs using their partner’s sperm to produce embryos).
Uterine abnormalities / Mullerian anomalies
Sometimes the uterus and fallopian tubes may not form like they should. These malformations are called Mullerian anomalies or defects. The main symptoms are the absence of periods and/or pain during sexual intercourse. The most common surgery is hysteroscopy to resect a uterine septum. Most women with this condition will have ovaries that produce eggs, meaning they can have children however they will need to use In-Vitro Fertilization (IVF) and a surrogate.
Free online tools for conception
Our experienced team has developed the following free tools for couples trying to conceive, to help you understand your fertility and chance of conception better:
- Ovulation Calculator: Maximise your chance of conceiving by ensuring you’re having sex at the right time with the Ovulation Calculator.
- Fertility Assessment Tool: This tool is designed to give you an indication of whether there are any factors that might be affecting your chance of falling pregnant and whether you should consider seeking the advice of a fertility specialist.
- Male Fertility Predictor: Use the Male Fertility Predictor tool to evaluate the male partner’s current fertility status given his lifestyle and common medical concerns.
When should we see a fertility specialist?
If you are over 35 and having trouble conceiving naturally, it’s important to seek medical advice within 6 months, as your egg quality and reserve has begun to decline. If you are under 35, we generally advise you to wait 12 months. In addition, if you have any known conditions such as a history of STD's or male factor issues, then don't delay in seeking Specialist help.
If you know or suspect a gynaecological condition or a male fertility issue could be contributing to pregnancy delay, we recommend making an appointment to see a Fertility Specialist.
Some fertility problems can be easily fixed with the right conception advice, lifestyle changes or even minor surgery – not all patients will require IVF. Whatever pathway to pregnancy you take, thanks to advances in reproductive technology, fertility treatment and other forms of assisted conception now offer a much higher chance of success.
First appointment overview and costs
A Queensland Fertility Group Specialist can assist with diagnosing gynaecological conditions, and identifying the best course of treatment to help you get pregnant. All our doctors are expert gynaecologists – so even if you are not trying to conceive, our specialists can help.
The initial consultation for a couple to see a Fertility Specialist varies from $220 – 350, and Medicare will reimburse approximately $95.00. For more information or to book a consultation with your preferred specialist, fill out the form below.
Typically, during a first appointment your specialist will assess your medical history, and will most likely recommend investigations such as blood tests (many of these are bulk billed) and an ultrasound scan. It is recommended your partner attends the consultation as well. The results of these will help you and your Fertility Specialist determine the best next steps for your individual circumstances. You should feel comfortable in this first appointment to mention any concerns you may have and ask questions.
If you are having trouble falling pregnant, a Queensland Fertility Group Fertility Specialist can help with investigations and treatment. All of our doctors are expert gynaecologists and/or obstetricians who have undertaken additional training and specialise in fertility.
If you would like to book an appointment, please call 1800 111 483 or fill out the form below.